ACLS Bradycardia Algorithm
Version control: This document is current with respect to 2015 American Heart Association Guidelines for CPR and ECC. These guidelines are current until they are replaced on October 2020. If you are reading this page after October 2020, please contact ACLS Training Center at support@acls.net for an updated document.
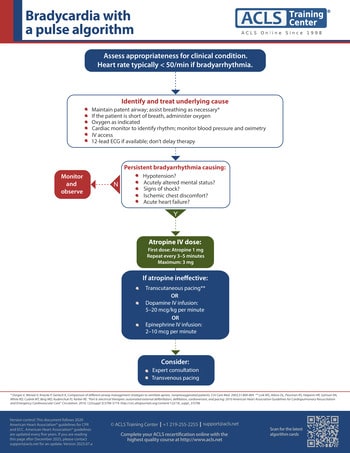
Using the ACLS Bradycardia Algorithm for Managing Bradycardia
The ACLS Bradycardia Algorithm outlines the steps for assessing and managing a patient who presents with symptomatic bradycardia. It begins with the decision that the patient's heart rate is < 60 bpm and that is the reason for the patient’s symptoms.
Steps
- Decision: Heart rate is < 60 bpm and is symptomatic.
- Assess and manage the patient using the primary and secondary surveys:
- Maintain patent airway.
- Assist breathing as needed.
- Administer oxygen if oxygen saturation is less than 94% or the patient is short of breath
- Monitor blood pressure and heart rate.
- Obtain a 12-lead ECG.
- Review patient's rhythm.
- Establish IV access.
- Complete a problem-focused history and physical exam.
- Search and treat possible contributing factors.
- Answer two questions to help you decide if the patient's signs and symptoms of poor perfusion are caused by the bradycardia (see Figure 2).
- Are the signs or symptoms serious, such as hypotension, pulmonary congestion, dizziness, shock, ongoing chest pain, shortness of breath, congestive heart failure, weakness or fatigue, or acute altered mental status?
- Are the signs and symptoms related to the slow heart rate?
- There may be another reason for the patient’s symptoms other than the slow heart rate.
- Decide whether the patient has adequate perfusion. The treatment sequence is determined by the severity of the patient's clinical presentation.
- If perfusion is adequate, monitor and observe the patient.
- If perfusion is poor, move quickly through the following actions:
- Prepare for transcutaneous pacing. Do not delay pacing. If no IV is present pacing can be first.
- Consider administering atropine 0.5 mg IV if IV access is available. This may be repeated every 3 to 5 minutes up to 3mg or 6 doses.
- If the atropine is ineffective, begin pacing.
- Consider epinephrine or dopamine while waiting for the pacer or if pacing is ineffective.
- Epinephrine 2 to 10 µg/min
- Dopamine 2 to 10 µg/kg per minute
Progress quickly through these actions as the patient could be in pre-cardiac arrest and need multiple interventions done in rapid succession: pacing, IV atropine, and infusion of dopamine or epinephrine.
Comments